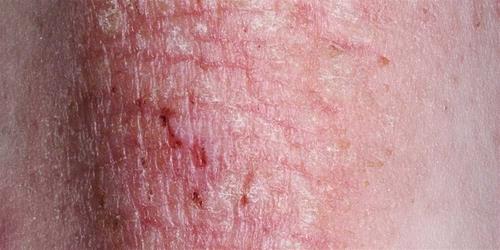
What is Eczema?
Eczema is a chronic inflammatory skin condition which causes areas of skin to become dry, hot, itchy, red and even cracked. It is sometimes called dermatitis or atopic eczema.
Epidemiology of Eczema
Eczema is the most common inflammatory skin condition in the world. It affects 20% of children in Ireland and 3% of adults. Therefore, 85% of children grow out of it and few go on to have lifelong eczema. The onset of eczema typically occurs before 12 months of age. Infants often suffer from eczema of the face, neck and trunk while older children are more commonly affected at the flexural and extensor surfaces of the arms and legs.
It is thought that earlier and more effective management of eczema is important in helping children to 'grow out of' their eczema.
What causes Eczema?
Eczema is caused by a combination of many factors including genetic predisposition to both skin barrier impairment and immune system activation. Environmental triggers and stress can play a role. Imbalance of the lipid matrix can compromise the skin barrier which leads to increased permeability and reduced skin antimicrobial function. It is known that inherited glycoprotein abnormalities in the skin barrier can play a role in some severe cases.
Research indicates that the immune system plays a significant role in eczematous disease. Eczema can be exacerbated by co-existing allergies both in terms of its extent, its severity and the number of eczema flares. This makes it particularly important to exclude common allergies to achieve the best clinical outcomes in the management of eczema.
What Is Atopy?
Atopy refers to the tendency in a person towards having eczema, asthma and hay fever. It is characterised by an overactive IgE mediated immune response to environmental factors. The same factors or triggers have no effect on the skin or airways of a non-atopic person.
Atopy is primarily genetically inherited which means that atopy runs in families. Despite this, some children from atopic families never develop eczema, asthma or hay fever. Furthermore, children with no family history of atopy can suffer from any of these atopic conditions.
What makes the skin drier in Eczema?
Chronically dry skin is a sign of impaired skin barrier function. Therefore, any external factors that make the skin drier can make eczema more difficult to manage:
- Low Humidity (e.g. air-conditioning).
- Hot or cold weather conditions (see climate section below).
- Washing and bathing too frequently or using very hot water / hard water / soaps.
- Chlorine in swimming pools.
How to maintain skin moisture in Eczema:
- Moisturise daily and always after bathing.
- Limit showers or baths to once per day and try to make them brief.
-
Use a soap substitute such as Silcocks Base or Cetaphil.
What factors can worsen Eczema?
Irritant triggers in Eczema
Most eczema sufferers are aware that certain substances irritate their skin and may even trigger an eczema flare. Eczematous skin is far more vulnerable to irritants such as:
- Coarse fibres in clothes (wool & synthetic)
- Harsh clothing detergents
- Soaps, make-up, perfumes and creams
- Dusty environments
How to limit the impact of irritants in Eczema:
- Clothes detergents:
- use fragrance free and non-biological detergents
- reduce the amount of detergent used if possible
- ensure clothes are well rinsed after washing
- If using soap to wash your hands, rinse off thoroughly.
- Wear protective clothing and gloves when handling detergents and cleaning chemicals.
- Limit the use of skin products (except those prescribed for eczema).
Allergic triggers in Eczema
Both an individual's genetics and their environment contributes to their risk of developing eczema, its severity and the response to treatment. If an allergy is identified as contributing to exacerbations of eczema then removal of the allergen from the affected patient's environment will result in improved eczema control. Immunotherapy desensitisation treatment is available for those who suffer from either house dust mite or pollen allergies.
Climate triggers in Eczema
Environmental conditions can have a big impact on eczema.
- The cold and damp conditions we experience in Ireland during winter may cause eczema to become more resistant to treatment. Dehumidifiers may be beneficial for asthma but can further exacerbate dry skin.
- During the summer months eczema often improves. This is caused by the departure of the colder weather and the increased exposure to UV light which has beneficial effects in moderation. Sunburn should always be avoided.
- In a small number of eczema patients sunlight will worsen their eczema. This is called photosensitive eczema.
- Moving to a new house or new area can have a beneficial or detrimental effect on eczema.
- Most people with eczema will become itchier and have redder skin when they are hot.
How to reduce the impact of a challenging climate
- Use superfine natural fibre clothing and bedding to reduce sweating and keep the skin cool.
- Keep the temperature cool and even throughout the house.
- Keeping cool in hot weather is important. Use a fan or even air conditioning if necessary. Having short cool showers will help.
Stress triggers in Eczema
It is well known that physical, psychological and social stress can act as triggers for eczema flares.
- Physical stress includes any medical illness e.g. the common cold.
- Psychological stress such as work stress or bereavement.
- Social stress such as moving house, changing school or family conflict.
Eczema itself may be the source of stress. It can cause significant discomfort which can lead to missing school or work. In addition, for some patients it can be a major cosmetic concern which leads to further stress.
Management of Eczema
Avoidance of irritants in Eczema
It is important to minimise exposures to any obvious aggravating factors. This includes irritants such as soaps, shower gels, detergents and fabrics which can be harsh on the skin. Silcock’s Base and Cetaphil are gentle non fragranced alternatives to soap. Consider washing newly bought clothing with a non-biological detergent to remove any remaining traces of dye. Heat can aggravate eczema and trigger itching. Ensure to avoid excessive clothing and blankets and use cotton rather than wool. Keep your house temperature under 20 degrees during the day and try to keep the bedroom at about 15 degrees overnight.
Avoidance of allergic triggers in Eczema
Allergies to common airborne allergens such as house dust mite, pollen and pet dander (cat, dog etc) can exacerbate eczema. It is therefore important to take avoidance measures in those who also suffer from these allergies. Immunotherapy to desensitise suffers of house dust mite or pollen allergy may be considered for those with significant eczema.
Food allergy should be considered in babies with widespread eczema which is completely unresponsive to treatment.
Pseudoallergy: Junk foods contain additives and preservatives which can worsen eczema in some children and adults. This is due to the stimulatory effect of these ingested chemicals on the immune system.
Emollients for Eczema
Daily use of a thick fragrance free complex moisturiser is recommended for eczema sufferers. Some patients require application more than once per day. Certain people will find some moisturisers more effective than others so it is useful to experiment with different brands.
Bathing and Cleaning in Eczema
Although a short daily bath is recommended, patients and parents can adjust the bathing routine based on experience. Keep the water temperature below 30 degrees. The addition of a 1-2 capfuls of bath emollient such as Oilatum is recommended. It is particularly important to moisturise after bathing.
In infants and young children ensure to clean around their mouths after eating using a soft wet towel. A thick moisturiser can then be reapplied to the area.
Medical Treatment of Eczema
It is important to quickly control eczema flare ups when they occur. This is because it is easier to get on top of exacerbations early on. It will also help to avoid the vicious cycle which can occur involving itching, scratching, potentiation of inflammation and potentially infection.
It is recommended to use a sufficiently strong steroid cream or ointment for flare ups. Gentler steroid creams are used for the face while stronger steroid creams are required for treatment of the hands and feet. Avoid being too sparing and apply the steroid cream or ointment in sufficient quantities just as you would with a suncream. Ensure to apply to all affected areas including broken skin and remove any skin flakes prior to application.
Always seek medical advice before using steroid creams on your children.
Does eczema increase the risk of food allergies?
Individuals who have eczema with elevated blood IgE levels are more likely to suffer from food allergies or allergies to environmental factors such as grass pollen, animal dander and house dust mites. Research indicates that the skin barrier dysfunction that occurs in eczema increases the risk of food allergy. Primary sensitisation is more likely to occur when new allergens are introduced through inflamed eczematous skin rather than the gastrointestinal tract.
It is therefore important that parents avoid introducing new foods, especially nuts and shellfish, during any acute exacerbation of eczema. It is also prudent to avoid eating nuts in the presence of an eczematous infants before they have been weaned on to nuts.
Contact Us to Schedule Your Consultation
If eczema is impacting your quality of life, schedule an appointment for assessment and personalised treatment.
Contact us today to arrange your appointment with one of our specialist allergy doctors.
Eczema Information for Health Professionals
The role of allergy in atopic dermatitis (AD) is complex. Atopic dermatitis is a chronic inflammatory condition of the skin with the hallmark feature of skin barrier dysfunction further worsened by inflammation and scratching. A more permeable skin barrier results in transepidermal water loss but it is likely that it also acts as a potential portal for developing allergen sensitisation and thus allergic disease. Indeed, atopic dermatitis is frequently the initial manifestation of atopy and allergic disease.
It has become apparent that the development and severity of atopic dermatitis involves a multifactorial process with genetic, environmental and inflammatory factors.
Genetic predisposition towards a defective skin barrier
Evidence suggests a strong genetic predisposition for atopic dermatitis. Twin studies found monozygotic twins had a 7-fold increased risk of developing atopic dermatitis versus a 3-fold in dizygotic twins.
Genes encoding for structural proteins in the skin are likely to play a role in the resultant defective skin barrier. Filaggrin protein is key to the development of a healthy skin barrier. Multiple mutations causing loss of function in the gene encoding for Filaggrin protein have been identified and these show a strong association with the development of atopic dermatitis. One such study found 63% of mutation carriers developed eczema by 3 years old.
These Filaggrin gene mutations are carried by at least 9% of Europeans but will not always confer disease. Indeed, 55% of those possessing filaggrin heterozygosity do not develop atopic dermatitis and Filaggrin mutations were only identified in 30% of patients with eczema in Europe.
Interestingly, independent of atopic dermatitis, having a Filaggrin gene mutation was found to be associated with an increased risk to developing asthma.
What role does the Immune System play in eczema?
The adaptive immune response evolves to become more robust and more specific during the first six months of life. The two main types of T Helper lymphocytes, Th-1 and Th-2, generally operate in a state of equilibrium. It has been found in atopic dermatitis that an imbalance often exists with a far greater number of Th-2 cells and their associated cytokine messengers. Genetic factors responsible for encoding cytokines involved in the regulation of IgE synthesis have been identified in atopic dermatitis. This genetic predisposition can result in a polarizing Th2 immune response with Th2 cytokines released (IL-4, IL-5 and IL-13) which favour IgE production resulting in mast cell hyperactivity and thus inflammation. In addition, many of these patient have high levels of Immunoglobulin E (IgE) antibodies and eosinophils.
In addition, these Th2 associated cytokines reduce antimicrobial properties of the skin precipitating bacterial and/or fungal colonization, altering their microbiome and furthering damage to the skin barrier. This causes the skin to become more vulnerable to penetration by
- Irritants such as soap, detergent, dirt
- Allergens such as house dust mite, pollen, animal dander and microbes
Langerhans cells are the specialised macrophages that reside in the epidermis. In atopic dermatitis, they become activated by irritants and allergens and signal dermal T cells to produce an even greater Th2 response. This further impairs skin barrier function which allows heavier bacterial and fungal colonisation of the skin. The skin becomes more vulnerable to infection and infections can become more difficult to control.
What is the role of IgE sensitisation in eczema?
The genetic predisposition to have a dysfunctional skin barrier and a dysregulated Th2 immune response in atopic dermatitis create the perfect environment for allergen sensitisation.
The initial presentation of early onset atopic dermatitis appears to be in the absence of IgE-mediated allergen sensitisation. However, within a short period of time, sensitisation occurs with elevation of total IgE alongside specific IgE antibodies to environmental allergens such as house dust mite, pollens and animal dander. In fact, it has been shown that approximately 80% of those with eczema have specific IgE sensitisation to at least one environment allergen.
Individuals with a history of pre-school atopic dermatitis are more likely to be polysensitised which increases with age. Interestingly a filaggrin mutation without a history of pre-school AD did not show a strong association with IgE sensitisation to foods and aeroallergens further corroborating the requirement for a defective skin barrier to allow the penetration of allergens and resultant sensitisation.
Furthermore, young children with atopic dermatitis are significantly more likely to be sensitised to foods including egg, milk, wheat, sesame, peanut and cod. In addition, children with a history of pre-school AD, particularly more severe and persistent AD, show a strong association with IgE sensitisation to food and aeroallergens.
In addition, approximately 25% of patients with atopic dermatitis have IgE sensitisation to self-proteins. It is suspected that pruritis causing intense scratching releases intracellular proteins from keratinocytes and endothelial cells inducing IgE autoantibodies. This autoimmunity further promotes inflammation.
Is Eczema associated with Food Allergy, Asthma and Allergic Rhinitis?
IgE sensitisation does not necessarily correlate with the development of an allergy or allergic disease.
Nevertheless, a strong association has been shown between having atopic dermatitis and having a food allergy. A Danish study demonstrated that 14.8% of atopic dermatitis patients had a challenge-confirmed food allergy although 90% of individuals (healthy and with AD) with confirmed food allergy had atopic dermatitis. This further highlights the link between atopic dermatitis and the development of food allergy.
On the other hand, children with atopic dermatitis before age 4 years have been found to be twice as likely to develop asthma in later childhood. Indeed 30-50% of children with atopic dermatitis will proceed to developing asthma while 35% will develop allergic rhinitis.
Is Anti-IgE therapy effective in eczema?
Despite the co-existence of atopic dermatitis with IgE sensitisation and allergic disease, there is less conclusive evidence for anti-IgE therapy, allergen avoidance measures and food elimination diets in the management of atopic dermatitis.
A number of trials for the use of Omalizumab (Anti-IgE therapy) in atopic dermatitis did not demonstrate it to be effective. However, more recently the ADAPT trial for a paediatric cohort with severe atopic dermatitis, atopy and high total IgE levels found a reduction in symptom severity with improved quality of life. A much greater improvement has been shown with Dupilumab (Anti-IL4 therapy) and systemic immunosuppressants such as Ciclosporin.
Is it beneficial to avoid aeroallergens in eczema?
Evidence has shown worsening of atopic dermatitis symptoms following exposure to aeroallergens in IgE sensitised AD patients. However, despite expectations, allergen avoidance measures for aeroallergens have so far shown limited benefit. This further highlights the complex relationship between atopic dermatitis and allergy.
Are food elimination diets effective in eczema?
There is only weak evidence to support elimination diets for eczematous individuals with suspected food allergy and IgE sensitisation. Nevertheless, some benefit for egg elimination in infants with egg allergy and sensitisation was shown.
Does the microbiome has an impact on Eczema?
The impact of the microbiome on atopic dermatitis has come under increased scrutiny of late. Exacerbations of eczema are accompanied by Staphylococcus aureus proliferation in the affected skin and a reduction in cutaneous microbiome diversity with fewer cutibacteria and malassezia yeasts than are present on normal skin. This is important because it is thought that the microbiome contributes to inflammatory immune responses in the skin. Researchers report that emollients increases biodiversity in eczematous skin.
The functions of microbial components of the skin flora are of particular interest to researchers. Areas such as the elbows, knees and axilla have higher moisture and humidity levels and consequently attract different microbiomes. It is hypothesized that different organism profiles found in different areas of the body might be responsible for the characteristic distribution of atopic dermatitis.
Other triggers of Eczema exacerbations
Irritant Exposure and Contact Allergens
There are multiple irritants that can aggravate atopic dermatitis including physical irritants such as wool and chemical irritants such as hygiene products, cosmetics or bleaches. Environmental irritants such as traffic exhaust fumes and cigarette smoke is likely to aggravate atopic dermatitis. In addition, atopic dermatitis carries an increased risk of co-morbid allergic contact dermatitis which can contribute to pruritis and stinging and burning of the skin. Allergens can include nickel, lanolin and fragrance mix. If suspected, patch testing may be considered.
Infection and colonization
The majority of atopic dermatitis patients are colonized by staphylococcal aureus which triggers inflammation via superantigen toxins, enhanced T cell activation and expression of IgE anti-staphylococcal antibodies. This in turn increases IL-31 expression driving pruritis. Scratching further encourages S. aureus binding. In addition this may cause an imbalance in the diversity of the skin microbiome further exacerbating atopic dermatitis. Furthermore, there is increased vulnerability to fungal and viral infections of the skin which can contribute. A source of bacteria is cream/ointment containers where 50% are contaminated.
Psychosocial factors
Psychological factors can have an impact on atopic dermatitis. Emotional stress and comorbid psychosomatic disease have been shown to be a factor in eliciting exacerbations of eczema. Psychological factors can also influence the itch-scratch cycle.